 |
 |
| J Cerebrovasc Endovasc Neurosurg > Volume 19(2); 2017 > Article |
|
Abstract
Carotid artery dissection is a significant cause of stroke in young patients. It may be asymptomatic and go undiagnosed, or minimal transient manifestations may follow, commanding a higher index of suspicion than ordinarily exists to avoid misdiagnosis. Reported herein is a 27-year-old man who suffered extracranial internal carotid artery dissection while practicing a Brazilian Jiu-Jitsu submission maneuver. The patient's condition suddenly deteriorated one week later due to distal embolization and stroke. Despite endovascular treatment, with stenting of the cervical carotid artery, neurologic deficits remained. Of note, the objective in martial arts, which is to kill or incapacitate, has yet to be fully tempered in transitioning to sport. Brazilian Jiu-jitsu, a relatively new and fast-growing form of martial art, places emphasis on submission maneuvers. Related injuries are not common knowledge and are poorly described in the literature. This account is intended to shed light on the risk of this discipline. Through education and improved supervision, vascular injuries of this nature and the potentially lethal or disabling consequences may thus be prevented in young athletes.
Although carotid artery dissection is implicated in only 2.5% of all strokes,3) it is among the leading causes of stroke in patients < 45 years old.3)5)10)23) In terms of the various cervical vascular injuries chronicled in the literature that are due to blunt trauma, sports-related events are almost entirely confined to case reports or limited case series. Brazilian Jiu-Jitsu is a specific style of martial art that has gained popularity in recent years.20)21) There is little actual documentation as yet, but the submission maneuvers that are practiced may predispose to certain injuries.21) This report describes a circumstance in which internal carotid artery dissection was directly attributable to a Brazilian jiu-jitsu maneuver.
A previously healthy 27 year-old professional male Brazilian jiu-jitsu fighter presented to the emergency room with headache, right motor deficit, and aphasia, all commencing 16 hours earlier. The patient had experienced a bout of severe neck pain one week earlier while practicing a submission maneuver known as the Rear Naked Choke or Lion Killer, with persistent pain locally thereafter. No family history of arterial dissection, stroke, connective tissue disorders, or migraine was elicited. The patient never smoked but the use of anabolic steroids (nandrolone and trenbolone) 1 month beforehand was reported.
Upon admission, findings included a Glasgow Coma Scale score of 11, right central facial paralysis, aphasia, and disproportionate right hemiparesis (muscular strength: right upper limb, grade 1/5; right lower limb, grade 3/5). There were no external signs of cervical trauma, such as bruising or abrasions.
Emergency computed tomography scan showed hypodensity in the left cerebral hemisphere (Fig. 1A). Due to the nature of trauma sustained and a clinical suspicion of dissection, conventional cerebral angiography was performed on an emergency basis, using a Berenstein 5F diagnostic catheter (Merit Medical Systems Inc., South Jordan, UT, USA) over a Radiofocus Guide wire 0.035 inch × 260 cm (Terumo Corp., Tokyo, Japan). Subsequently, decreased filling of the left middle cerebral artery, with several thrombotic occlusions of M2 and M3 segments (Fig. 2A), and a dissection narrowing the origin of left internal carotid artery were observed (Fig. 2B). The hydrophilic guidewire was positioned in the left external carotid artery, enabling replacement of the diagnostic catheter by an Epsylar 6F introducer sheath (OptiMed, Ettlingen, Germany), which was introduced into distal common carotid artery as a guiding catheter. A 5 mm Spider embolic protection device (ev3 [Covidien], Plymouth, MN, USA) was opened within left internal carotid artery, and angioplasty was done, deploying a Protégé RX self-expanding stent 6-8-40 mm (ev3 [Covidien]) to cover the entire length of the dissection (Fig. 2C, D). The procedure was uneventful, using heparin for the duration, followed by acetylsalicylic acid (200 mg/day) and clopidogrel (75 mg/day) in the intensive care unit. Intracranial thrombolysis was not attempted.
During the first day of hospitalization, level of consciousness declined (Glasgow Coma Scale score, 8), calling for tracheal intubation. Another emergency computed tomography scan showed left hemispheric infarction, with hemorrhagic transformation and midline shift. An intraparenchymal catheter was implanted to monitor intracranial pressure and over the next 24 hours conservative measures were done, including mannitol, hypertonic saline infusion, induced hypothermia, pentobarbital coma therapy and moderate short term hyperventilation. However, despite all efforts, high intracranial pressure forced a decompressive craniectomy. On admission, routine laboratory testing for inflammatory, rheumatic, coagulation disorders had excluded other causes of ischemic stroke. Electrocardiography and transesophageal echocardiography showed no cardiac embolic source.
Severe pneumonia ultimately ensued, accompanied by extensive pleural effusions. Bilateral chest drainage was required, as well as eventual right pulmonary decortication. Nevertheless, the patient did recover (Glasgow Coma Scale score, 11) and was discharged after 3 months with a tracheostomy, gastrostomy, and persistence of prior deficits (modified Rankin Scale score, 4). A 2-day re-hospitalization was needed 5 months later for cranioplasty, inserting an acrylic plate (Fig. 1B). One year later, physical therapy was still in progress (Glasgow Coma Scale score, 15; modified Rankin Scale score, 3). The patient walked with paretic gait due to right-sided weakness (muscular strength: right upper limb, grade 2/5; right lower limb, grade 4/5) and was dysphasic. He retired as a result of his handicaps.
In the realm of martial arts, cervical vascular dissection typically involves the vertebral artery, having been reported with mixed martial arts,20) karate,19) wrestling,4) judo,9) kickboxing,11) and kung-fu.17) Although carotid artery dissection has also been described in taekwondo,18) karate14) and mixed martial arts,13) direct bodily impact (i.e., kicks and punches) may be responsible, which is not characteristic of Brazilian jiu-jitsu. As such, vulnerability of the extracranial carotid artery may reflect a tethering effect on the prepetrosal segment (at skull base entry), in conjunction with free neck mobility.8) On the other hand, this particular dissection involved the origin of internal carotid artery, suggesting the following biomechanical sequence: 1) carotid artery compression, creating a point of fixation and 2) subsequent hyperextension of the neck, with contralateral head rotation.22) The resultant traction would suffice to stretch and rupture the intimal layer of carotid artery distal to its point of fixation (Fig. 3).
Carotid injury due to blunt cervical trauma may pose a diagnostic challenge. Symptoms are sometimes absent, minimal and transient, or even delayed for up to 12 months after the insult.5) The primary cause of stroke is embolic,1)2)3) which explains the delay between injury and onset of neurologic deficits both here and in a similar incident with Taekwondo.18) Embolism likely results from localized thrombosis of disrupted endothelium.12)
Despite inherent challenges, early diagnosis of cervical arterial dissection improves patient prognosis.2) This patient scenario underscores the imperative for neurosurgeons and other sports physicians to consider arterial dissection when evaluating symptomatic athletes. Headache and neck pain are common, and pain may be the only indication.8) Other signs and symptoms are cranial nerve palsy, Horner's syndrome, pulsatile tinnitus, ataxia, vertigo, and dizziness.2)4) However, given the frequency of asymptomatic carotid stenosis, patients with risk factors who practice contact sports should be screened for this condition as well.14)
A thorough history is fundamental, but because the diagnosis is confirmed through imaging, early studies may be prudent in this patient subset.2)4) Still, there is no consensus on imaging at present. Kerwin et al.7) advocate liberal screening of patients suffering blunt trauma and presenting with neurologic deficits, massive epistaxis, and cranial or spinal fractures. Doppler ultrasound and magnetic resonance or angiotomography are less invasive alternatives, whereas conventional angiography enables endovascular treatment and is thus preferable.2)8) Unfortunately, this athlete failed to seek help at the onset of pain, when a rapid and inexpensive carotid duplex scan may have prevented the life-threatening sequelae that were suffered.
Overall mortality in this setting is 3-4%, with satisfactory outcomes in ~75% of survivors through conservative therapy.7) Prevention of stroke is the treatment goal; so despite the lack of randomized controlled trials, early anticoagulation is advised to halt the succession of new neurologic deficits.2) However, evidence of symptomatic thromboembolic intracranial vascular occlusion and major stroke are contraindications for anticoagulation, according to Biondi et al.,1) posing a risk of hemorrhagic transformation. Stent-assisted endovascular repair was therefore warranted here, rather than anticoagulation. Emergency stenting also serves to stabilize the intimal flap and deter potential deterioration precipitated by emboli.22) Thrombolysis of intracerebral occlusions in an acute phase is also a safe and effective option, even following extracranial carotid artery stenting.15) It was contraindicated in this patient since he was beyond the 6-hour time window and had major involvement (over one-third) of the territory supplied by middle cerebral artery, heightening the risk of intracerebral hemorrhage.6)
We acknowledge that no sport is considered completely safe, and the martial arts especially have evolved over millennia expressly as means to kill and disable.16) The transition to sport is a recent phenomenon that appears to be lacking in safety standards and regulations.16) Arterial dissection is a potentially devastating and underrecognized problem in these healthy young enthusiasts.2)4)7) Awareness of the risks must be increased and better supervision implemented to prohibit prolonged or overly vigorous moves.12)21) Coaching and training staff must also caution participants against a sense of immunity, urging prompt medical attention for injuries sustained. A grasp of potential consequences is critical in preventing such injuries, helping as well to raise the index of suspicion, prompt earlier and accurate diagnosis, and thus improve outcomes.12)
References
1. Biondi A, Katz JM, Vallabh J, Segal AZ, Gobin YP. Progressive symptomatic carotid dissection treated with multiple stents. Stroke. 2005 9;36(9):e80-e82;


3. Bogousslavsky J, Pierre P. Ischemic stroke in patients under age 45. Neurol Clin. 1992 2;10(1):113-124;


4. Gupta V, Dhawan N, Bahl J. Minor trauma causing stroke in a young athlete. Case Rep Neurol Med. 2015 3;2015:182875.




5. Hauser V, Zangger P, Winter Y, Oertel W, Kesselring J. Late sequelae of whiplash injury with dissection of cervical arteries. Eur Neurol. 2010 64(4):214-218;


6. Jauch EC, Saver JL, Adams HP Jr, Bruno A, Connors JJ, Demaerschalk BM, et al. Guidelines for the early management of patients with acute ischemic stroke: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2013 3;44(3):870-947;


7. Kerwin AJ, Bynoe RP, Murray J, Hudson ER, Close TP, Gifford RR, et al. Liberalized screening for blunt carotid and vertebral artery injuries is justified. J Trauma. 2001 8;51(2):308-314;


8. Kim YK, Schulman S. Cervical artery dissection: pathology, epidemiology and management. Thromb Res. 2009 4;123(6):810-821;


9. Lannuzel A, Moulin T, Amsallem D, Galmiche J, Rumbach L. Vertebral-artery dissection following a judo session: a case report. Neuropediatrics. 1994 4;25(2):106-108;



10. Lyrer P, Engelter S. Antithrombotic drugs for carotid artery dissection. Stroke. 2004 2;35(2):613-614;


11. Malek AM, Halbach VV, Phatouros CC, Mayers PM, Dowd CF, Higashida RT. Endovascular treatment of a ruptured intracranial dissecting vertebral aneurysm in a kickboxer. J Trauma. 2000 1;48(1):143-145;


12. McCarron MO, Patterson J, Duncan R. Stroke without dissection from a neck holding manoeuvre in martial arts. Br J Sports Med. 1997 12;31(4):346-347;



13. McClain R, Wassermen J, Mayfield C, Berry AC, Grenier G, Suminski RR. Injury profile of mixed martial arts competitors. Clin J Sport Med. 2014 11;24(6):497-501;


14. Meairs S, Timpe L, Beyer J, Hennerici M. Acute aphasia and hemiplegia during karate training. Lancet. 2000 7;356(9223):40.


15. Mishra A, Stockley H, Goddard T, Sonwalker H, Wuppalapati S, Patankar T. Emergent extracranial internal carotid artery stenting and mechanical thrombectomy in acute ischaemic stroke. Interv Neuroradiol. 2015 4;21(2):205-214;



16. Oler M, Tomson W, Pepe H, Yoon D, Branoff R, Branch J. Morbidity and mortality in the martial arts: a warning. J Trauma. 1991 2;31(2):251-253;


17. Pacei F, Valvassori L, Bet L. Vertebral artery dissection during Kung-Fu training. Neurol Sci. 2014 2;35(2):331-332;



18. Pary LF, Rodnitzky RL. Traumatic internal carotid artery dissection associated with taekwondo. Neurology. 2003 4;60(8):1392-1393;


19. Pentore R, Nichelli P. De-afferented state syndrome (locked-in syndrome) following sudden cervical sprain trauma during a karate training session. Riv Neurol. 1991 Mar-Apr;61(2):66-70;

20. Slowey M, Maw G, Furyk J. Case report on vertebral artery dissection in mixed martial arts. Emerg Med Australas. 2012 4;24(2):203-206;


21. Scoggin JF 3rd, Brusovanik G, Izuka BH, Zandee van Rilland E, Geling O, Tokumura S. Assessment of injuries during Brazilian Jiu-Jitsu Competition. Orthop J Sports Med. 2014 2;2(2):2325967114522184.



Fig. 1
Computed tomography scan imaging: (A) at emergency admission, showing hypodensity of left cerebral hemisphere after “windowing and leveling” and (B) at postoperative cranioplasty (B).

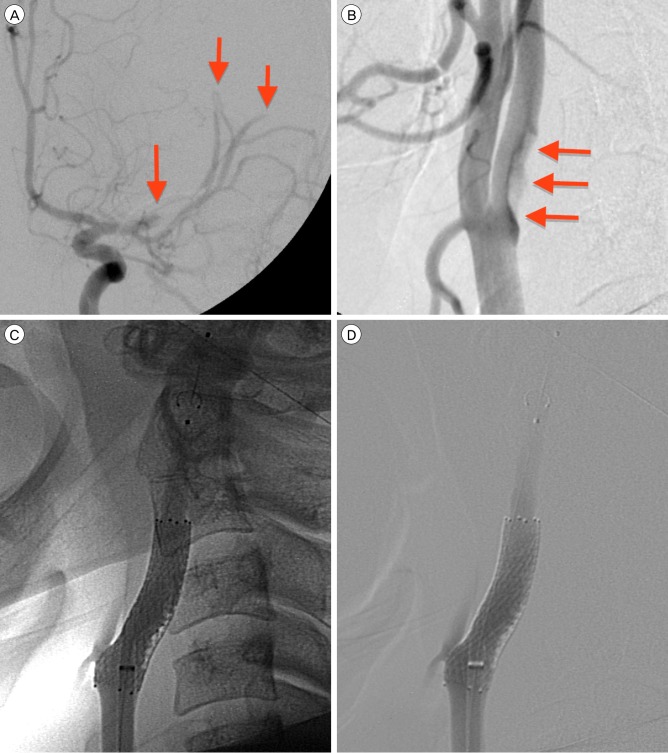
Fig. 2
Cerebral angiogram: (A) anteroposterior view of occluded M2 middle cerebral artery segments (arrows); (B) left common carotid artery in lateral view, showing narrowing at internal carotid artery origin (arrows); (C) stent placement; and (D) postoperative control images confirming adequate arterial patency, with mural compression of thrombus.
- TOOLS
-
METRICS

-
- 7 Crossref
- 0 Scopus
- 3,526 View
- 33 Download
- Related articles
-
Internal Carotid Artery Trunk Aneurysms - Management and Outcome.2006 June;8(2)
Trans-radial Carotid Artery Stenting in a Patient with Abdominal Aortic Occlusion2016 June;18(2)





 PDF Links
PDF Links PubReader
PubReader Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC Download Citation
Download Citation Print
Print



