 |
 |
| J Cerebrovasc Endovasc Neurosurg > Volume 23(4); 2021 > Article |
|
Abstract
Inadvertent flow alterations in the parent artery during microsurgical clipping might produce postoperative ischemic complications. Intraoperative recognition of such alterations and its correction might improve operative outcomes in these patients. We present the case of a thirty-five-year-old male with an incidental small left anterior choroidal aneurysm. Microsurgical clipping induced an external compression of the anterior choroidal artery against the posterior clinoidal process which was identified in situ through surgical exploration and the loss of arterial doppler signal in the vessel. After failed attempts at clip repositioning, a posterior clinoidectomy was performed to decompress the artery. This resulted in arterial flow recovery. The aneurysm was successfully treated, and a severe ischemic complication was likely avoided. This intraoperative phenomenon has not yet been described in the literature.
Treatment of anterior choroidal artery (AChA) aneurysms remains a challenging task due to the artery’s complex anatomy and vascular distribution. Frequent ischemic complications have been reported with devastating consequences [1,6,7,10]. Occasionally, unnoticed flow alterations in the parent artery due to microsurgical clipping have resulted in postoperative ischemic complications [3]. On-site recognition of such alterations and their correction might improve operative outcomes in these patients.
We present a case of an AChA aneurysm which developed flow impairment in the parent artery during surgical clipping due to compression against a prominent posterior clinoid process.
A thirty-five-year-old male with a history of chronic headaches was referred for neurosurgical evaluation due to the incidental finding of a small left AChA saccular aneurysm (Fig. 1A, B). The patient’s past medical history was positive for arterial hypertension, smoking and a history of aneurismal subarachnoid hemorrhage in the family. Conservative management vs. treatment alternatives were discussed, and the patient opted for surgery. Due to the aneurysm’s broad neck, surgical clipping was favored over endovascular coiling.
The patient was positioned supine in the operating table with the head fixed with a Mayfield clamp, slightly elevated from the level of the right auricula. Positioning was completed with slight extension and a 20-degree rightward head rotation. A mini-pterional craniotomy was performed (Fig. 1C). The proximal sylvian fissure was split and the carotid cistern dissected. A brain retractor was positioned to elevate the frontal lobe with gentle retraction. The optic nerve (ON) and internal carotid artery (ICA) were identified. At the origin of the AChA, on the posterolateral aspect of the ICA, the aneurysm was observed (Fig. 1D). The origin of the AChA was identified on the anterior aspect of the aneurysm sac. The neck of the aneurysm was dissected, and clipping was performed with a 7 mm straight Yasargil permanent clip (Aesculap, Braun GmbH, Frankfurt, Germany) (Fig. 1E). The arterial doppler microprobe (Mizuho Medical, Tokyo, Japan) was brought into the operative field (Fig. 1F), and an absence of flow in the AChA was noticed. After clip removal, the doppler probe was used again, and robust flow in the AChA was found. A new slight curved 6.5 mm clip was applied, and the maneuver again resulted in sonographic signs of flow impairment.
After careful exploration, the surgeon realized that the absence of flow within the artery was due to a direct compression of the AChA against the posterior clinoidal process (PCP). Several attempts were made to reposition clips with different settings (straight, slight curved, curved, angled tip) to avoid the arterial compression, but they proved to be unsuccessful. A posterior clinoidectomy with a Kerrison rongeur was then performed. This maneuver allowed for free movement of the AChA, with the arterial compression subsiding (Fig. 1G, H). Flow restoration was verified with a new doppler sonographic control. Fig. 2 shows the operative field after the definitive clipping and an artistic illustration of the procedure. The patient had no neurological deficits postoperatively and was discharged on day 3 of the hospital admission.
The treatment of AChA aneurysms remains challenging, not only because of the complexity of the vascular anatomy and the small caliber of the AChA, but also because of the fearsome ischemic complications derived [1,4,6,8,11]. Previous reports describe the risk of AChA territory ischemia at 12-16% [2,3,5,6,9].
Among the causes for AChA ischemic complications are: unintentional clipping resulting in arterial occlusion [3,9], thromboembolism due to temporary clipping of a parent vessel and arterial kinking due to clip rotation [5]. Ischemic complications were previously noted even with preserved arterial diameter. The presence of atheromatous plaques on the aneurysm neck may also be a cause of AChA occlusion [2]. For this reason, intraoperative monitoring techniques should be performed to ensure that the blood flow within the artery remains patent [5]. Intraoperative angiography with intravenous indocyanine green (ICG) or micro-doppler ultrasound are useful tools that surgeons can use to avoid ischemic complications [9].
During the case presented, vascular anatomy seemed to be preserved but an absence of flow in the AChA was noticed. The in situ identification of a mechanical compression of the parent artery and the ulterior surgical decompression, likely prevented a devastating ischemic complication. Of note, the PCP is rarely involved in AChA compression. However, in this case, a very prominent PCP, in association with a closely located trajectory of the supraclinoid ICA, could have favored this rare intraoperative event.
To the best of our knowledge, there are no reports in the literature of direct external compression of the AChA against the PCP induced by aneurysm clipping.
We present the case of an external clip-induced AChA compression against the PCP during aneurysm surgery. This phenomenon has not been described in the literature before. A posterior clinoidectomy proved to be effective in restoring normal flow in the AChA after several attempts at clip repositioning failed.
Fig. 1.
(A) CT angiography with bone reconstruction (lateral view): an aneurysm arising in the left AChA is observed. Inferiorly and medial to the aneurysm, the PCP with two bony prominences projecting superiorly and posteriorly. (B) Superior view of the same CT angiography. (C) Exposure of the sylvian fissure via a mini-pterional approach. (D) Surgical view under the operative microscope after the carotid cistern was dissected. The aneurysm sac was exposed and the origin of the AChA was identified. The PCP is medial to the aneurysm. (E) Intraoperative image of the clipped aneurysm, the compression of the AChA against the PCP is evidenced. (F) Use of Doppler probe on the AChA, which showed absence of flow. (G) Posterior clinoidectomy using Kerrison rongeur. (H) AChA liberated after the posterior clinoidectomy. CT, computed tomographic; AChA, anterior choroidal artery; PCP, posterior clinoid process; An, aneurysm; KR, kerrison rongeur.
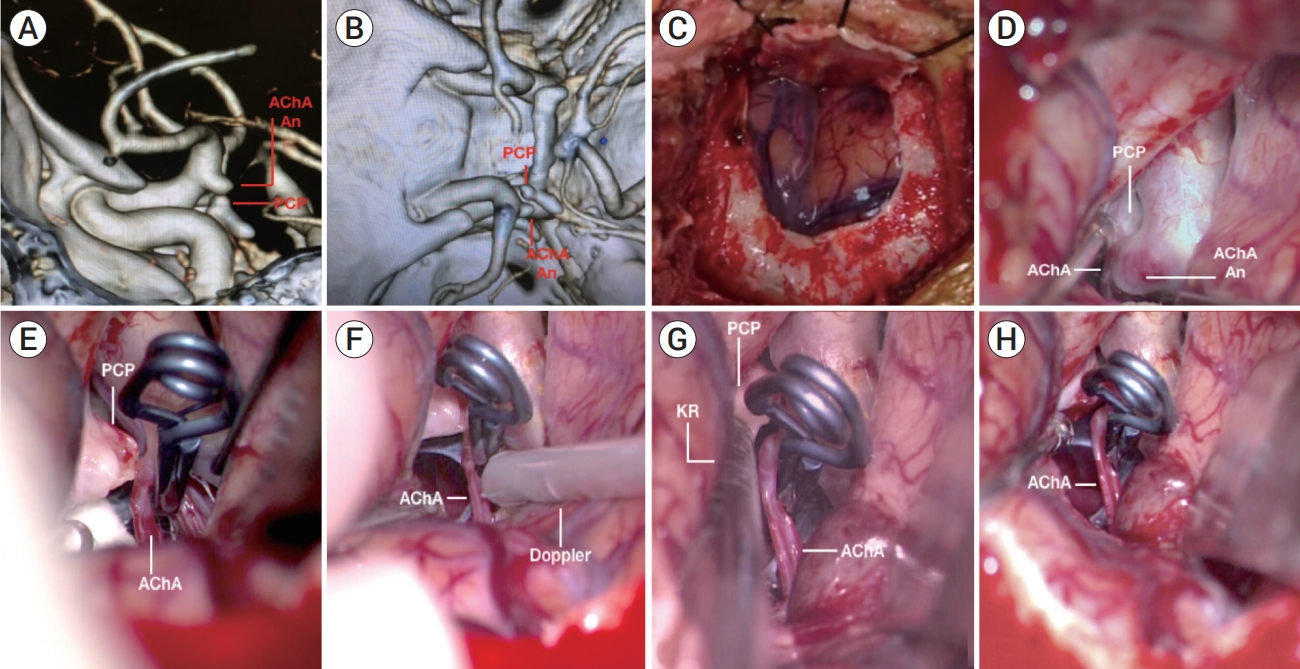
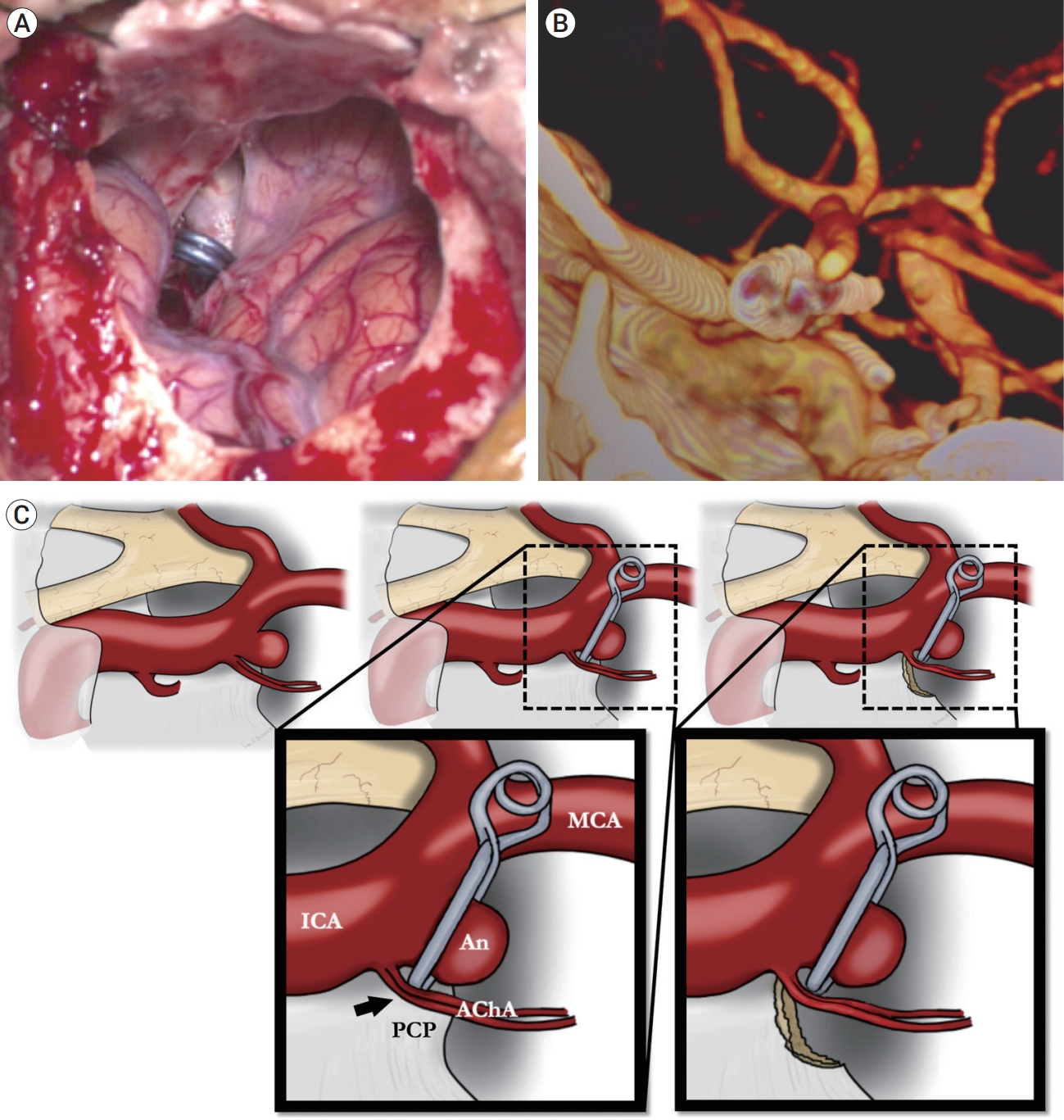
Fig. 2.
(A) Macroscopic view of the surgical field after aneurysm clipping and posterior clinoidectomy. (B) Post-surgical CT angiography showing the clip and its projection in the space previously occupied by the superior projection of the PCP. (C) Artistic illustration of the concept detailed in the present report (the black arrow points at the site of vascular compression of the AChA against the PCP). CT, computed tomographic; PCP, posterior clinoid process; An, aneurysm; AChA, anterior choroidal artery; ICA, internal carotid arter; MCA, middle cerebral artery.
REFERENCES
2. Bohnstedt BN, Kemp WJ 3rd, Li Y, Payner TD, Horner TG, Leipzig TJ, et al. Surgical treatment of 127 anterior choroidal artery aneurysms: a cohort study of resultant ischemic complications. Neurosurgery. 2013 Dec;73(6):933-9.


3. Cho MS, Kim MS, Chang CH, Kim SW, Kim SH, Choi BY. Analysis of clip-induced ischemic complication of anterior choroidal artery aneurysms. J Korean Neurosurg Soc. 2008 Mar;43(3):131-4.



4. Drake CG, Vanderlinden RG, Amacher AL. Carotid-choroidal aneurysms. J Neurosurg. 1968 Jul;29(1):32-6.


5. Felbaum D, Zhao DY, Nayar VV, Kalhorn CG, McGrail KM, Mandir AS, et al. Real-time evaluation of anterior choroidal artery patency during aneurysm clipping. Cureus. 2016 Feb;8(2):e495.



6. Friedman JA, Pichelmann MA, Piepgras DG, Atkinson JL, Maher CO, Meyer FB, et al. Ischemic complications of surgery for anterior choroidal artery aneurysms. J Neurosurg. 2001 Apr;94(4):565-72.


7. Hupperts RM, Lodder J, Heuts-van Raak EP, Kessels F. Infarcts in the anterior choroidal artery territory. Anatomical distribution, clinical syndromes, presumed pathogenesis and early outcome. Brain. 1994 Aug;117(Pt 4):825-34.


8. Kim BM, Kim DI, Shin YS, Chung EC, Kim DJ, Suh SH, et al. Clinical outcome and ischemic complication after treatment of anterior choroidal artery aneurysm: comparison between surgical clipping and endovascular coiling. Am J Neuroradiol. 2008 Feb;29(2):286-90.



9. Shibata Y, Fujita S, Kawaguchi T, Hosoda K, Komatsu H, Tamaki N. Use of microvascular Doppler sonography in aneurysm surgery on the anterior choroidal artery. Neurol Med Chir (Tokyo). 2000 Jan;40(1):30-5.


- TOOLS
-
METRICS

-
- 0 Crossref
- 0 Scopus
- 2,461 View
- 62 Download
- ORCID iDs
-
Juan Santiago Bottan

https://orcid.org/0000-0002-7126-4682 - Related articles



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC Download Citation
Download Citation Print
Print



