 |
 |
| J Cerebrovasc Endovasc Neurosurg > Volume 23(3); 2021 > Article |
|
Abstract
Blood Blister-like aneurysms are intracranial non-saccular aneurysms with higher rupture risk due to its fragile wall. Diagnosis is performed in the acute phase of a subarachnoid hemorrhage. There are several treatment options based on reconstructive or deconstructive techniques. This paper aims to discuss the limitations of microsurgery clipping for a ruptured blister aneurysm. We report on a case of a female patient presented with a Fisher III subarachnoid hemorrhage. Cerebral angiography revealed an internal carotid artery blister aneurysm. Initially microsurgery clipping was successfully performed. However, after a few days the patient presented new subarachnoid hemorrhage. The new cerebral angiography showed growth of the previously clipped aneurysm, with displacement of the clip from the position adjacent to the artery. High-flow bypass was performed obtaining definitive treatment. This is a definitive approach for blister aneurysms. If microsurgery clipping is chosen, a strict follow-up is required due to the dynamic nature of this lesion and the chance of re-bleeding even after successfully clipping.
Blood Blister-like aneurysms (BBAs) correspond to 0.5-2% of all intracranial aneurysms [1,3]. They usually are small (<2 mm), broad-based lesions, with fragile wall, that more frequently occur in the supraclinoid segment of internal carotid artery (ICA). Despite being uncommon, they have a higher rupture risk when compared to saccular aneurysms (SA). Unlike saccular aneurysm that could be discovered incidentally, BBAs are diagnosed in the acute phase after a subarachnoid hemorrhage (SAH) and because of their fragility wall and dynamic nature, treatment is challenging. In general, treatment is based in deconstructive or reconstructive methods that could be performed through microsurgery or endovascular interventions [13].
This paper aims to discuss the limitations of reconstructive treatment through microsurgery clipping in a patient with subarachnoid hemorrhage due to a ruptured BBAs.
A 58-year-old female patient presented to Emergency Department (ED) complaining of severe headache, nausea and vomiting. She evolved with impaired consciousness level, Glasgow coma scale (GCS) of 14 at admission, no cranial nerve palsy and no other neurological deficits and so classified with Hunt Hess II. Past medical history was significant only for arterial hypertension. She was monitored at intensive care unit (ICU).
Brain computed tomography (CT) revealed a diffuse SAH occupying basal cisterns and classified as Fisher III. 3D Angio-CT reconstruction did not reveal any alterations. Digital subtraction angiography (DSA) was performed and revealed a small broad-based aneurysm at supraclinoid segment of the ICA suggestive of blister aneurysm (BBA) (Fig. 1).
A neurosurgical procedure was performed with right pterional craniotomy and microsurgical dissection of the basal cisterns, after proximal carotid control in the cervical region. Exposure of the supraclinoid carotid revealed a small broad-based aneurysm at the dorsal wall of the internal carotid artery, covered by fibrin. After temporary proximal and distal clipping, the blister aneurysm was clipped with a straight clip, involving the fibrin in the clip (Fig. 2). Microsurgical clipping was performed without any complication and complete occlusion of the lesion through microscopic view. Five days after the procedure, patient was still in ICU for neurological observation and blood pressure control, she remained conscientious, with GCS 15. However, she evolved with decreased level of consciousness, facial central paralysis and left hemiparesis. Brain CT revealed new hemorrhage and other DSA was performed showing growth of the previously clipped aneurysm, with the clip distancing from the artery wall (slip clip) (Fig. 3).
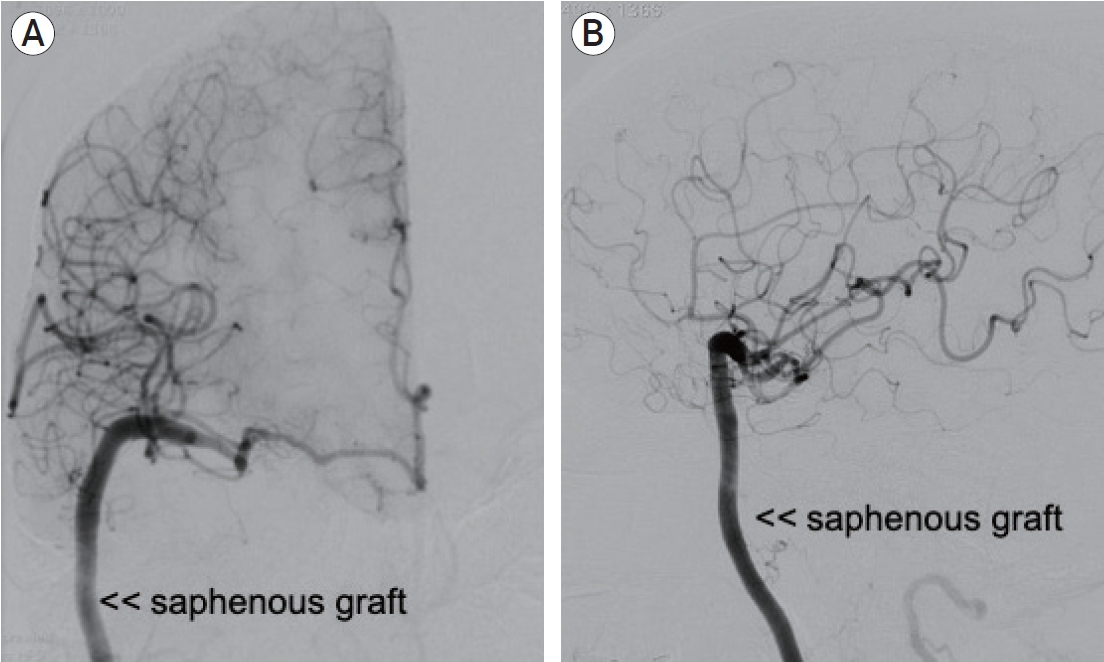
In this scenario it was realized a high-flow bypass with interposition of saphenous vein. The ICA was occluded on the neck and also in the supraclinoid segment, right after the aneurysm. During microsurgery it was noticed that the lesion grew again and push the clip. The procedure occurred without complication and control angiography showed good patency of the anastomosis (Fig. 4). She was discharge one month after the initial subarachnoid hemorrhage without any neurological sequel and a GOS of 5.
Intracranial aneurysms constitute a high morbidity and mortality condition in neurosurgery practice [6,7]. They are more common diagnosed after SAH, however could also be incidentally discovered specially in patients with familial history. Saccular aneurysms are the most common type. BBAs are a rare and special type of non-saccular aneurysm. Its incidence varies among series, however they usually are discovered after SAH and correspond to 0.5-2% of all ruptured intracranial aneurysm [20].
They most commonly arise from the dorsal wall of the ICA-supraclinoid segment. Considering all ICA aneurysm, they correspond to 0.9-6.5%. They are small broad-based lesions that resemble an ulcer, with a fragile wall that is more associated to high rupture risk when compared to saccular aneurysms [10]. Some studies considered that its pathology is associated to an arterial dissection. Ruptured BBAs consist of a platelet plug covering a thin layer of adventitia, which overlies a defect in the intima and media that lacks the usual collagen layer [5].
The angio-CT has an elevated rate of false negative, as in this case, and angiography is the gold-standard for diagnosis and required for follow-up, specially when reconstructive procedures are performed [2]. The most recent works also highlight the importance of repeat angiogram even if the initial exam does not reveal any alteration, but there is a high suspicion [19]. They could appear after because of usually they are very small and have a dynamic behavior [9,12,17].
Treatment could be performed through microsurgery, using different techniques such direct clipping, trapping, wrapping and bypass, or through endovascular interventions, by a variety of techniques like balloon-assisted coil embolization, stent-assisted coil embolization, parent vessel occlusion or stent flow diversion [8,10,11]. It is remarkable that rupture risk during any intervention is high and surgeon may be prepared for this situation. Considering endovascular treatment, several approaches are possible, such as occlusion, coiling and flow diverter [11].
Reconstructive or deconstructive procedures [16] could be performed through microneurosurgery. In the former, the normal flow patency is preserved and in the latter one it is provoked an interruption of the regular arterial flow and the segment of the vessel that contain the aneurysm is excluded of circulation [4].
Direct aneurysm clipping is associated to lesser morbidity because the artery patency maintenance, nevertheless this type of vascular lesion has a dynamic behavior and despite success in surgery, complications may occur such in the case reported. Perfect clipping was obtained, however it was insufficient to block flow through the lesion and so grew back. The force through its fragile wall surpassed the strength of the clip and push it and so rebled occurred. Fortunately, this event was not catastrophic and was diagnosed soon during observation in ICU and angiography was performed and revealed a slip clip [14].
In this scenario a deconstructive procedure was proposed. Despite high-flow bypass can cause cerebral ischemia due to exclusion of a segment of the ICA and so greater neurological morbidity, it represents a definitive treatment. No blood flow pass over the lesion and so there is no risk of further bleeding. In this patient the collateral circulation was sufficient to maintain a proper cerebral vascularization and so no ischemia occurred.
A natural history of BBAs generally is catastrophic [18]. There are some reports in which the authors opted only for observation and in seriated angiography the lesion disappeared, however it could be seen as an exception of its generally behavior. Intervention is the best choice because of if other hemorrhage occur could be fatal. The current tendency of treatment defends more aggressive procedures excluding this aneurysm of circulation through deconstructive methods [15]. This paper highlights the importance of considering this type of procedure as initial treatment.
BBAs are rare vascular lesions diagnosed after the occurrence of a subarachnoid hemorrhage. Despite is uncommon in neurosurgical practice, their particularities should be known aiming a proper diagnosis and treatment. Angiography is the gold-standard exam inasmuch as Angio-CT has a great index of false negative. Its therapeutic approach is difficult because of they have a dynamic behavior due to its fragile wall. Deconstructive procedures such as microsurgical high-flow bypass, despite of having a great morbidity is a definitive treatment that is associated to high rate of cure compared to clipping since its intrinsic nature can push out the clip even after a succeed occlusion.
Fig. 1.
Pre-operative ICA angiogram showing a small broad-based aneurysm (arrow) at dorsal wall of the ICA. (A) Unsubstracted image. (B) 3D rotational angiography reconstruction. ICA, internal carotid artery.
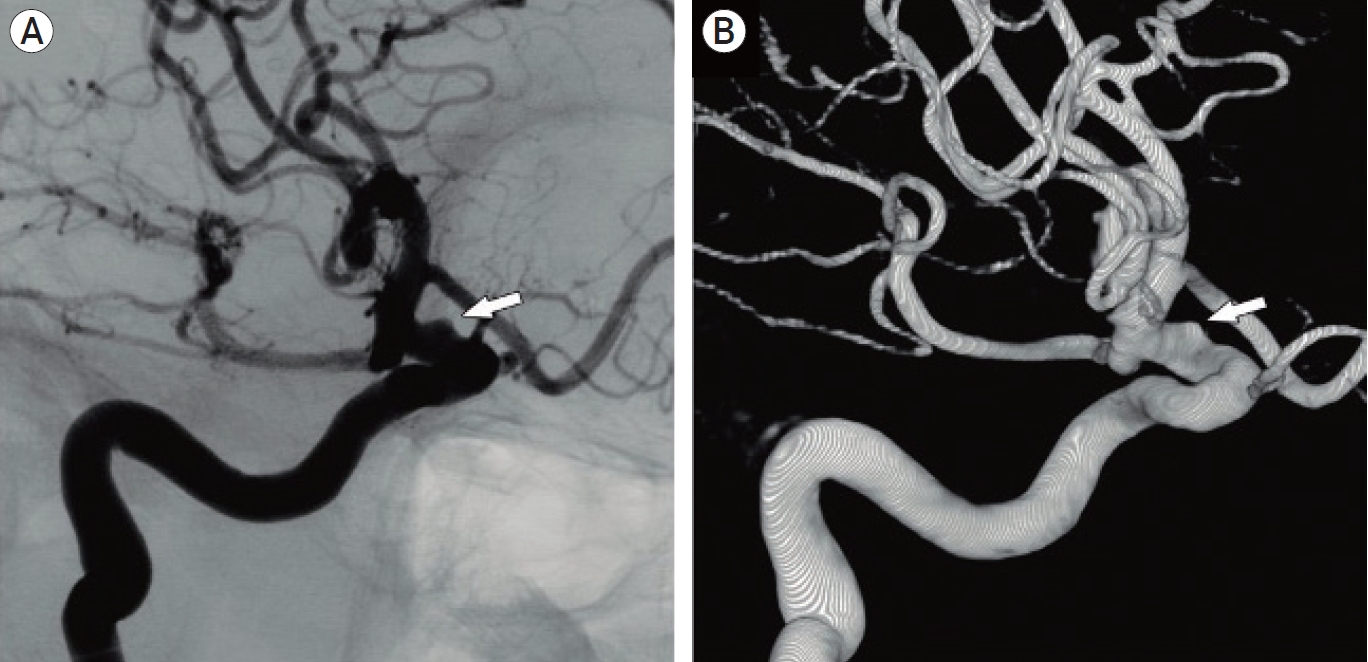
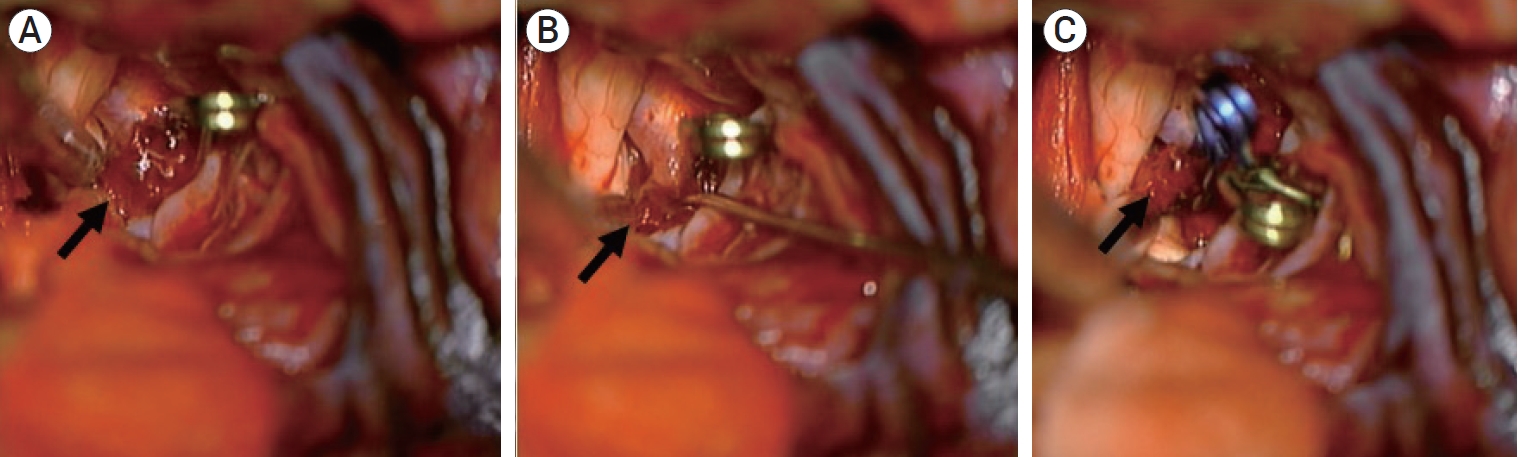
Fig. 2.
Microsurgical image after temporary clipping of the proximal (extracranial) and distal internal carotid artery. (A) The blister aneurysm covered by fibrin (arrow) is observed. (B) After partial removal of fibrin, it is possible to observe the blister aneurysmal neck (arrow). (C) After definite clipping.
REFERENCES
1. Bojanowski MW, Weil AG, McLaughlin N, Chaalala C, Magro E, Fournier JY. Morphological aspects of blister aneurysms and nuances for surgical treatment. J Neurosurg. 2015 Nov;123(5):1156-65.


2. Coutinho JM, Sacho RH, Schaafsma JD, Agid R, Krings T, Radovanovic I, et al. High-Resolution Vessel Wall Magnetic Resonance Imaging in Angiogram-Negative Non-Perimesencephalic Subarachnoid Hemorrhage. Clin Neuroradiol. 2017 Jun;27(2):175-83.


3. Gonzalez AM, Narata AP, Yilmaz H, Bijlenga P, Radovanovic I, Schaller K, et al. Blood blister-like aneurysms: single center experience and systematic literature review. Eur J Radiol. 2014 Jan;83(1):197-205.


4. Hellstern V, Aguilar-Pérez M, AlMatter M, Bhogal P, Henkes E, Ganslandt O, et al. Microsurgical clipping and endovascular flow diversion of ruptured anterior circulation blood blister-like aneurysms. Interv Neuroradiol. 2018 Dec;24(6):615-23.



5. Indo M, Oya S, Tanaka M, Matsui T. High incidence of ICA anterior wall aneurysms in patients with an anomalous origin of the ophthalmic artery: possible relevance to the pathogenesis of aneurysm formation. J Neurosurg. 2014 Jan;120(1):93-8.


6. Ji T, Guo Y, Huang X, Xu B, Xu K, Yu J. Current status of the treatment of blood blister-like aneurysms of the supraclinoid internal carotid artery: A review. Int J Med Sci. 2017 Apr 8 14(4):390-402.



7. Lee CC, Hsieh TC, Wang YC, Lo YL, Lee ST, Yang TC. Ruptured symptomatic internal carotid artery dorsal wall aneurysm with rapid configurational change. Clinical experience and management outcome: an original article. Eur J Neurol. 2010 Oct;17(10):1277-84.


8. Mokin M, Chinea A, Primiani CT, Ren Z, Kan P, Srinivasan VM, et al. Treatment of blood blister aneurysms of the internal carotid artery with flow diversion. J Neurointerv Surg. 2018 Nov;10(11):1074-8.


9. Nakatomi H, Segawa H, Kurata A, Shiokawa Y, Nagata K, Kamiyama H, et al. Clinicopathological study of intracranial fusiform and dolichoectatic aneurysms: insight on the mechanism of growth. Stroke. 2000 Apr;31(4):896-900.


10. Park TJ, Kim KH, Cho JH. The blood blister like-aneurysm: usefulness of Sundt Clip. J Cerebrovasc Endovasc Neurosurg. 2017 Sep;19(3):171-83.



11. Peitz GW, Sy CA, Grandhi R. Endovascular treatment of blister aneurysms. Neurosurg Focus. 2017 Jun;42(6):E12.


12. Peschillo S, Missori P, Piano M, Cannizzaro D, Guidetti G, Santoro A, et al. Blister-like aneurysms of middle cerebral artery: a multicenter retrospective review of diagnosis and treatment in three patients. Neurosurg Rev. 2015 Jan;38(1):197-202; discussion 202-3.


13. Shigeta H, Kyoshima K, Nakagawa F, Kobayashi S. Dorsal internal carotid artery aneurysms with special reference to angiographic presentation and surgical management. Acta Neurochir (Wien). 1992 119(1-4):42-8.


14. Sorimachi T, Osada T, Hirayama A, Shigematsu H, Srivatanakul K, Matsumae M. Preservation of anterior choroidal artery blood flow during trapping of the internal carotid artery for a ruptured blood Blister-like aneurysm with highflow bypass. World Neurosurg. 2019 Feb;122:e847-55.


15. Strickland BA, Rennert RC, Bakhsheshian J, Ravina K, Fredrickson V, Giannotta SL, et al. Extracranial-intracranial bypass for treatment of Blister aneurysms: efficacy and analysis of complications compared with alternative treatment strategies. World Neurosurg. 2018 Sep;117:e417-24.


16. Wang L, Cai L, Qian H, Shi X. Overestimated role of extra-cranial-to-intracranial bypass in management of Blood-Blister aneurysm. World Neurosurg. 2018 Oct;118:391-2.


17. Xu D, Xie X, You C. Angiographic appearance of Pulsatile Blister aneurysm. World Neurosurg. 2018 Feb;110:371-2.


18. Zeineddine HA, Jones W, Conner CR, Simpson B, Blackburn S, Day AL. Spontaneous healing of a ruptured Blood Blister-like aneurysm. World Neurosurg. 2018 Nov;119:85-8.


- TOOLS
-
METRICS

-
- 0 Crossref
- 0 Scopus
- 2,218 View
- 65 Download
- ORCID iDs
-
Guilherme Brasileiro de Aguiar

https://orcid.org/0000-0003-3206-2081 - Related articles




 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC Download Citation
Download Citation Print
Print



