 |
 |
| J Cerebrovasc Endovasc Neurosurg > Volume 17(3); 2015 > Article |
|
Abstract
We describe a case of a huge intramural hematoma in a thrombosed middle cerebral artery aneurysm. A 47-year-old female patient with liver cirrhosis and thrombocytopenia presented to the neurosurgical unit with a 5-day history of headache and cognitive dysfunction. Magnetic resonance imaging and computed tomography of the brain showed a thrombosed aneurysm located in the right middle cerebral artery with a posteriorly located huge intramural hematoma mimicking an intracerebral hematoma. Imaging studies and cerebrospinal fluid analysis showed no evidence of subarachnoid hemorrhage. Angiography showed a partially thrombosed aneurysm at the origin of the right anterior temporal artery and an incidental aneurysm at the bifurcation of the right middle cerebral artery. Both aneurysms were embolized by coiling. After embolization, the thrombosed aneurysmal sac and intramural hematoma had decreased in size 4 days later and almost completely disappeared 8 months later. This is the first reported case of a nondissecting, nonfusiform aneurysm with a huge intramural hematoma, unlike that of a dissecting aneurysm.
Intracranial aneurysm is frequently associated with intramural hematoma. Few cases have been previously reported, particularly in association with fusiform or dissecting aneurysm. We report on a unique case of a nondissecting, nonfusiform aneurysm with a huge intramural hematoma, unlike that of a dissecting aneurysm.
A 47-year-old female patient was admitted to our hospital with a few hours history of personality change, cognitive dysfunction, and headache. She also had a 12-year history of abortion and thrombocytopenia. She was drowsy, with a Glasgow coma scale of 14. The platelet count was markedly decreased to 58,000/µL, and physical examination showed splenomegaly. Computed tomography (CT) of the abdomen showed a cirrhotic liver with splenomegaly. However, she had no history of hepatitis. Lumbar puncture was performed after platelet transfusion, and no red blood cells were found in the cerebrospinal fluid.
Magnetic resonance (MR) imaging and CT of the brain were performed for evaluation of suspected intracranial lesions. A T1-weighted axial image showed a target-like thrombosed aneurysm located in the right anterior sylvian fissure (Fig. 1B). Ovoid high signal intensity was suggestive of a hematoma surrounding the posterior aspect of the aneurysm. A T2-weighted axial image also showed a thrombosed aneurysm and a posteriorly located hematoma with a surrounding dark line (Fig. 1A). Difference in signal intensity was observed between the posteriorly located hematoma and the thrombosed aneurysm on T1- and T2-weighted images, i.e. on T1- and T2-weighted images, the posterior hematoma showed homogeneous high signal intensity, whereas the thrombosed portion of the aneurysm showed intermediate and inhomogeneous high signal intensity (Fig. 1A, B). A gadolinium-enhanced axial image showed no definite enhancement of the lesions (Fig. 1C). On precontrast CT scan (Fig. 3A), the thrombosed aneurysm showed a highly attenuating wall. This high attenuation on CT images presented as high signal intensity on T1- and T2-weighted images. The posteriorly located hematoma abutted the aneurysmal sac. The hematoma also differed in density from the highly attenuating aneurysm wall. No evidence of subarachnoid hemorrhage was observed on MR or CT images. Digital subtraction angiography was performed, and 2 unruptured aneurysms were detected in the right middle cerebral artery (Fig. 2A, B).
Surgical intervention was not performed because of continued thrombocytopenia. Instead, coil embolization was performed immediately. After embolization, follow-up angiography showed faint staining of the contrast media on the capsule of the hematoma posterior to the thrombosed aneurysm (Fig. 2C, D). Immediately after coil embolization, follow-up CT of the brain showed capsular enhancement in the aneurysmal sac and the posterior hematoma (Fig. 3B). The aneurysmal sac and hematoma were decreased in size 4 days after coil embolization (Fig. 3C-E), and they had almost completely disappeared 4 months later (Fig. 3F). After 1 year, MR imaging of the brain showed that the hematoma in the right temporal lobe had completely disappeared (Fig. 1D, F). Ovoid high signal intensity suggestive of a hematoma abutted the posterior aspect of the aneurysm. A T2-weighted axial image also showed the thrombosed aneurysm and the posteriorly located hematoma with the surrounding dark line (Fig. 1A). Difference in signal intensity was observed between the posteriorly located hematoma and the thrombosed aneurysm on T1- and T2-weighted images, i.e. on T1- and T2-weighted images, the posterior hematoma showed homogeneous high signal intensity, whereas the thrombosed portion of the aneurysm showed intermediate and inhomogeneous high signal intensity (Fig. 1A, B). A gadolinium-enhanced axial image showed no definite enhancement of the lesions (Fig. 1C).
Despite their high prevalence and clinical importance, the pathogenetic mechanism of an intracranial aneurysm is complex and still not fully understood. Unlike the "usual" saccular type of aneurysm, giant partially thrombosed aneurysm is extremely rare, and its pathogenesis is still unclear. This report presents a case of subadvential hematoma in a saccular aneurysm. Intracranial aneurysms are frequently associated with intramural hematomas. Few cases have been previously reported, particularly in association with fusiform dissecting aneurysms.6)7)8)9)
Histological examination of thrombosed giant aneurysms performed by Yashi et al.7)9) found more fresh hemorrhages between old thrombus and aneurysmal wall with clefts of fresh blood, indicative of dissection of the aneurismal wall by blood flow. This hypothesis suggests that parent arterial flow is a factor for the growth of aneurysm and thrombus. However, it cannot explain our case due to its independence of a parent lumen and thrombosed intramural hematoma. According to a recent report by Krings et al.,3)4)5) the pathogenesis of partially thrombosed aneurysms can be explained by recurrences of subintimal dissection with subadventitial hemorrhages as well as sequential incomplete repairs. Suggested main intrinsic factors include the vasa vasorum, systemic disease, and segmental vulnerability. Krings et al.4)5) also suggested a mechanism by which proliferation of the vasa vasorum finally causes repeated subadventitial hemorrhages from the vasa vasorum, resulting in formation of intramural hematoma.
This case supports the hypothesis that proliferation of the vasa vasorum may contribute to the formation of a giant saccular aneurysm. Surgical intervention was not performed in our case because of the patient's thrombocytopenia. However, based on the ovoid hematoma abutting the aneurysmal sac observed on MR and CT images, curvilinear staining of the contrast media during the angiographic procedure (Fig. 1), and delayed capsular enhancement of the posterior hematoma on CT (Fig. 2), it is strongly suggested that the hematoma originated intramurally from the aneurysmal capsule. In addition, the hematoma was ovoid, well-defined, and confined within the sylvian fissure. These findings differed from those of subarachnoid hemorrhage observed on CT images. The patient showed no red blood cells in the cerebrospinal fluid. The aneurysms were not ruptured during angiography, and subarachnoid hemorrhage was not evident on MR or CT images.
This is the first reported case of a nondissecting, nonfusiform aneurysm with a huge intramural hematoma, which is morphologically different from a dissecting aneurysm. This case supports the hypothesis that proliferation of the vasa vasorum may contribute to the formation of a giant saccular aneurysm.
References
1. El Beltagy M, Muroi C, Imhof HG, Yonekawa Y. Peripheral large or giant fusiform middle cerebral artery aneurysms: report of our experience and review of literature. Acta Neurochir Suppl. 2008 103:37-44;


2. Horie N, Takahashi N, Furuichi S, Mori K, Onizuka M, Tsutsumi K, et al. Giant fusiform aneurysms in the middle cerebral artery presenting with hemorrhages of different origins. Report of three cases and review of the literature. J Neurosurg. 2003 8;99(2):391-396;


3. Krings T, Choi IS. The many faces of intracranial arterial dissections. Interv Neuroradiol. 2010 6;16(2):151-160;



4. Krings T, Lasjaunias PL, Geibprasert S, Pereira V, Hans FJ. The aneurysmal wall. The key to a subclassification of intracranial arterial aneurysm vasculopathies? Interv Neuroradiol. 2008 9;14(Suppl 1):39-47;

5. Krings T, Piske RL, Lasjaunias PL. Intracranial arterial aneurysm vasculopathies: targeting the outer vessel wall. Neuroradiology. 2005 12;47(12):931-937;



6. Mrak G, Paladino J, Stambolija V, Nemir J, Sekhar LN. Treatment of giant and large fusiform middle cerebral artery aneurysms with excision and interposition radial artery graft in a 4-year-old child: case report. Neurosurgery. 2014 3;10(Suppl 1):E172-E177; discussion E177



7. Nagahiro S, Takada A, Goto S, Kai Y, Ushio Y. Thrombosed growing giant aneurysms of the vertebral artery: growth mechanism and management. J Neurosurg. 1995 5;82(5):796-801;


Fig. 1
Initial T1-weighted axial image shows the target-like thrombosed aneurysm in the right anterior sylvian fissure (B). Another ovoid high signal intensity suggests hematoma surrounded by the posterior aspect of the aneurysm. T2-weighted axial image also shows the thrombosed aneurysm and posteriorly located hematoma with a surrounding dark line (A). The posteriorly located hematoma differs in signal intensity from the thrombosed aneurysm on T1- and T2-weighted images, i.e., the posterior hematoma shows homogeneous high signal intensity, whereas the thrombosed portion of the aneurysm shows intermediate and inhomogeneous high signal intensity on T1- and T2-weighted images (A, B). Gd-enhanced axial image shows no definite enhancement of the lesions (C). After one year, MR of the brain shows almost resorption state of the hematoma in the right temporal lobe.(D-F).
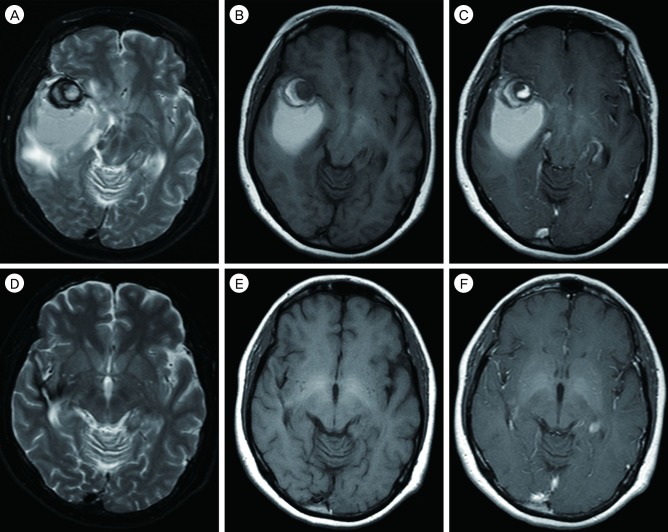
Fig. 2
Digital subtraction angiography was performed and two unruptured aneurysms were found in the right middle cerebral artery. (A, B) Surgical intervention was not performed due to continued thrombocytopenia. Instead, coil embolization followed immediately. After embolization of two aneurysms, follow-up angiography shows faint staining of the contrast

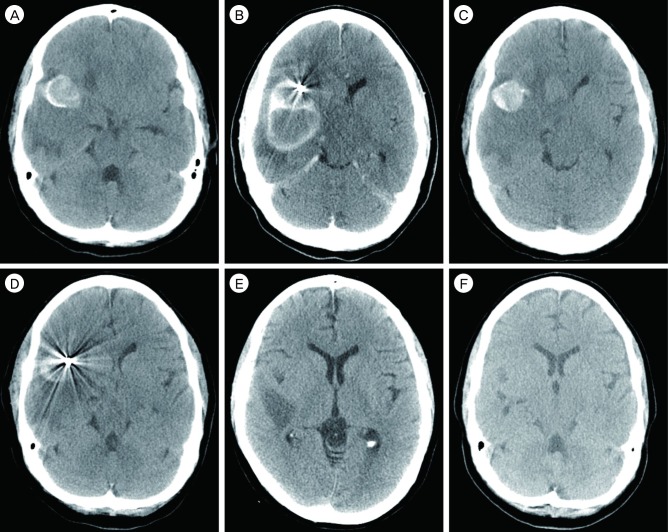
Fig. 3
On precontrast CT scan (A), the thrombosed aneurysm shows a high attenuating wall. The posteriorly located hematoma abuts the aneurysm sac. The hematoma also differs from the high attenuating aneurysm wall in density. Follow-up brain CT was performed immediately after coil embolization. Capsular enhancement is seen not only in the aneurysm sac but also in the posterior hematoma (B). (C-E) and F are CT images of the brain at POD 4 days, 11 days, 1 month, and 5 months. The aneurysm sac and hematoma had decreased in size 4 days after coil embolization (C-E) and almost disappeared 4 months later (F).
- TOOLS
-
METRICS

-
- 3 Crossref
- 0 Scopus
- 2,102 View
- 24 Download
- Related articles
-
Intra-aneurysmatic thrombectomy in a distal anterior cerebral artery aneurysm2023 December;25(4)
Microsurgical Anatomy of the Middle Cerebral Artery.2000 September;2(2)
Kissing Aneurysms of Distal Anterior Cerebral Arteries: A Case Report.2001 March;3(1)



 PDF Links
PDF Links PubReader
PubReader Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC Download Citation
Download Citation Print
Print



